+86 178 5514 5298
+86 178 5514 5298
Leave Your Message
-
 CONTACT NUMBER
CONTACT NUMBER -
 CONTACT NUMBER
CONTACT NUMBER -
 CONTACT NUMBER
CONTACT NUMBER



In the world of clinical diagnostics, the vacuum blood collection tube is an essential tool. Dr. Emily Carter, a leading expert in clinical laboratory technology, emphasizes, "The right tube can make all the difference in sample quality." This statement rings true as various types of vacuum blood collection tubes are tailored for specific tests and purposes.
Different tubes serve different functions, from serum separation to plasma collection. Each type is color-coded for easy identification, yet the confusion can arise when choosing the right one. Mistakes in tube selection can lead to compromised samples or inaccuracies in test results.
Understanding the top 10 types of vacuum blood collection tubes is vital for healthcare professionals. Each tube has unique features and uses, making it crucial to match them with specific tests. Salient details, like additives in certain tubes, play a significant role. Proper knowledge can elevate patient care, but many still overlook this vital aspect.

Vacuum blood collection tubes are crucial in modern healthcare. They come in various types, each serving specific purposes based on the tests conducted. Generally, these tubes contain different additives that facilitate blood preservation and testing accuracy. The most common types include EDTA tubes, used for hematology tests, and serum separator tubes, which are ideal for biochemistry tests. Each tube has unique specifications regarding volume, material, and color coding.
EDTA tubes, for instance, are typically purple-lid and hold around 4-5 mL of blood. They prevent clotting, making them essential for complete blood counts. Conversely, serum separator tubes, often orange or red, include gel to separate serum from blood after centrifugation.
Tips: Always confirm the type of test required before collecting blood. Each test might have different requirements. Proper tube selection can significantly reduce the chances of retesting. Moreover, ensure you understand the shelf life of the tubes and their storage conditions. Improper storage can lead to compromised results.
In some cases, professionals may overlook tube types. This can result in delays or inaccuracies in diagnosis. Paying close attention to specifics is vital for effective patient care. A common mistake is using the wrong tube, which can affect blood test results.
Blood collection tubes play a crucial role in laboratory diagnostics. Various additives in these tubes can significantly impact test results. These additives are essential for preserving blood samples and ensuring the accuracy of laboratory analyses. Common types include anticoagulants, clot activators, and gel separators.
Anticoagulants, like EDTA and citrate, prevent clot formation. They are vital for hematology tests. According to the Clinical Laboratory Standard Institute (CLSI), improper use of these additives can lead to skewed results. For example, EDTA can cause cellular distortion if not mixed adequately. Meanwhile, gel separators facilitate serum separation by forming a barrier during centrifugation. This ensures that serum does not contaminate cellular components. Such separation is critical for biochemistry tests.
Despite the advances in tube technology, challenges remain. The choice of tube and additive can vary based on the test type. This inconsistency may lead to confusion among healthcare providers. Some studies suggest that certain blood collection practices could introduce variation in test outcomes. Therefore, standardizing practices is essential for improving accuracy. Only through meticulous attention to detail can the full potential of blood collection tubes be realized.
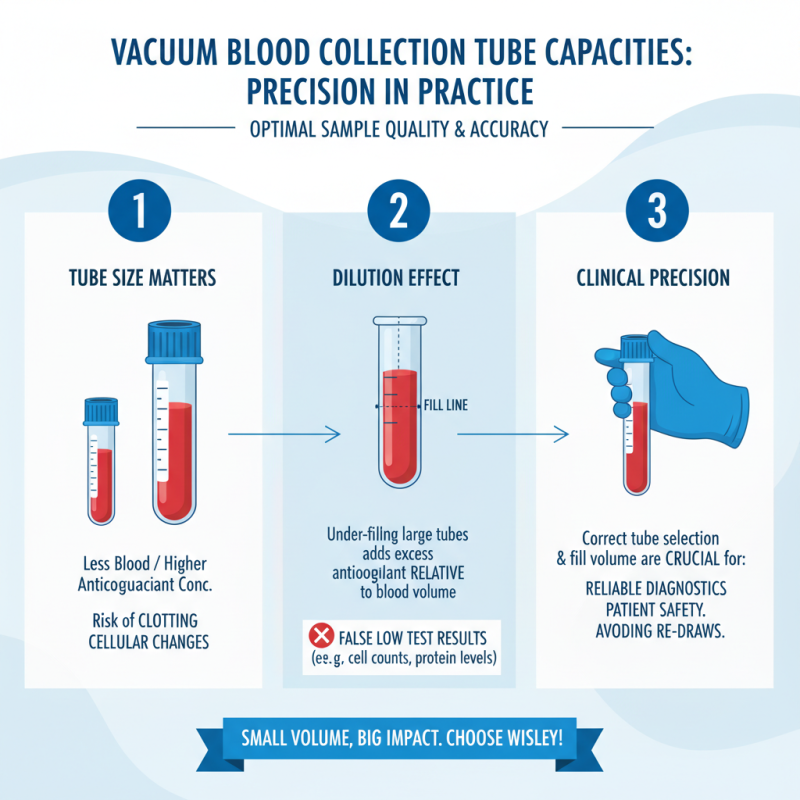
When working with vacuum blood collection tubes, understanding their capacities is essential. Different tube sizes can directly impact the quality of blood samples. For instance, larger tubes hold more blood, but they can also lead to dilution if not used correctly. This can result in inaccurate test results. In clinical settings, precision is crucial. A small misjudgment in volume can change everything.
Moreover, not all tests require the same amount of blood. Some tests, like certain biochemical assays, need specific tube capacities to ensure optimal mixing with additives. Insufficient blood can cause under-dilution, while too much blood may not activate preservatives properly. This complexity raises questions about how to standardize practices in various laboratories.
Errors can occur when technicians overlook tube specifications. This oversight may seem minor but can significantly affect patient outcomes. Inconsistent sample quality over time can compromise trust in laboratory results. Therefore, paying attention to tube selection and its influence on sample quality must be a priority in medical environments.
Choosing the right vacuum blood collection tube is crucial. Each tube type serves a specific purpose and can affect test results significantly. For instance, different additives like EDTA, citrate, or heparin are used to prevent clotting. According to a recent industry report, improper tube selection can lead to inaccurate test outcomes in up to 20% of cases.
Tips: Always confirm the required tube type for each test. This varies by laboratory protocols. Ensure you check any updates to guidelines, as they can change.
Blood collection often requires multiple tests. The tube's color indicates its additive. For example, red-top tubes typically contain no additives, while blue-top tubes contain citrate for coagulation studies. Make sure your team is aware of how to identify these tubes quickly. Misidentifying tubes is a common error that can delay results.
Tips: Use a color-coded chart in the collection area. This helps avoid mistakes.
Adherence to guidelines can improve efficiency. Yet, inconsistencies in training can lead to miscommunication. Regular training sessions are essential for maintaining accuracy in blood collection practices. It's important to reflect on the existing protocols and identify areas for improvement.
When selecting blood collection tubes, industry standards are crucial. Various organizations create guidelines to ensure safety and accuracy. For instance, guidelines often focus on material quality, sterility, and labeling. Compliance with these standards avoids dangerous outcomes and enhances test precision. The color of the tube often indicates the additive inside, which can affect laboratory results.
Regulatory considerations also impact the production of these tubes. Manufacturers must meet specific health and safety regulations. Many facilities emphasize the importance of regular inspections. However, some manufacturers overlook this due diligence. This negligence can result in subpar products reaching healthcare providers. Reacting to these lapses is essential for patient safety.
Quality assurance processes are another key aspect. Each batch of tubes should undergo rigorous testing. While many laboratories implement these protocols, some do not. This inconsistency raises questions about reliability. Clear documentation of these tests is vital for traceability. Addressing these flaws can improve the overall integrity of blood collection practices.